

MedFriendly®


Autonomic Dysreflexia
Autonomic dysreflexia is a life-threatening condition that
occurs in response to stimulation of internal organs
(such as an expanded bladder) or of the skin, after the
shock of a spinal injury has worn off. Specifically,
patients with this autonomic dysreflexia have a spinal
cord injury located near the middle of the spinal cord
(an area known as T7) or above. T7 (Thoracic 7) refers
to the 7th segment of the thoracic (chest) area of the
spine. Autonomic dysreflexia is characterized by an
impairment of the autonomic nervous system. If you
already know all about the autonomic nervous system,
then skip the next paragraph. If you don't know what the
autonomic nervous system is, then the second
paragraph was written just for you.
FEATURED BOOK: Autonomic Disorders: A Case Based Approach
WHAT IS THE AUTONOMIC NERVOUS SYSTEM?
The autonomic nervous system is an extensive network in the body (with connections to
the spinal cord) that is important for involuntary bodily functions that are necessary to
maintain life, such as respiration (breathing) and heart rate. The autonomic nervous
system consists of the sympathetic nervous system (the part that generally excites the
body by doing things such as increasing both the heart rate and blood pressure), and the
parasympathetic nervous system (the part that generally calms the body down by doing
things such as decreasing both the heart rate and blood pressure). Thus, the sympathetic
and parasympathetic nervous systems work in opposition to each other.
"Where Medical Information is Easy to Understand"™
WHAT ARE THE SIGNS & SYMPTOMS OF AUTONOMIC
DYSREFLEXIA?
In autonomic dysreflexia, the sympathetic and parasympathetic
nervous systems are activated at the same time, and this causes all
sorts of serious problems.
These serious problems include very high blood pressure, slow
heart rate, severe headaches, redness of the skin above the area
of the spinal cord injury, paleness of the skin below the area of the
spinal cord injury, sweating, and convulsions (severe, involuntary
muscle spasms).
As one can tell by reading this list of signs and symptoms, some are caused by activation of the excitatory
sympathetic nervous system (high blood pressure, severe headaches, redness of the skin, sweating, and
convulsions), whereas others are caused by the activation of the calming parasympathetic nervous
system (slow heart rate and paleness of the skin).
HOW IS IT THAT STIMULATION OF INTERNAL ORGANS OR THE SKIN CAN LEAD TO SUCH
SERIOUS PROBLEMS?
You may be wondering how it is that stimulation of internal organs or the skin can result in such serious
symptoms for patients with certain types of spinal cord injuries. When an internal organ or the skin is
stimulated, nerves receive this information below the area of the spinal cord injury. Keep in mind that the
autonomic nervous system is intact below the area of the spinal cord injury and it responds to the
stimulation by constricting (narrowing) tiny arteries. By making these tiny arteries narrower, the blood
pressure increases. This makes sense because it takes more pressure to move fluid through a narrow
space than a wide space.
The increased blood pressure is sensed by nerve endings that are designed to detect changes in blood
pressure. These nerve endings are located in the aorta (a large artery that comes out of the heart) and
the carotid sinus (an open area in the wall of the common carotid artery, where it splits in two). The
carotid sinus is located in the neck area. The nerve endings that detect the pressure send an "uh-oh"
message to the parasympathetic nervous system to calm things down. The parasympathetic nervous
system becomes activated and decreases the heart rate.
The problem is that the blood vessels in the internal organs and in other areas of the body do not widen to
decrease the blood pressure. Why? Because the messages sent by the parasympathetic nervous system
to do so cannot travel past the area where the spinal cord is damaged. It's like trying to send electricity
through a broken electrical wire...the electricity is only going to go so far. Because the body cannot
respond the way it should to decrease the blood pressure, the blood pressure stays elevated and the
body goes into crisis mode, with all sorts of contradictory responses happening at once.
WHY IS AUTONOMIC DYSREFLEXIA SO SERIOUS?
The reason that autonomic dysreflexia is so serious is because if it is not treated and brought under
control quickly, it can lead to constant and uninterrupted seizures (muscle spasms), stroke (a burst artery
or a blockage of an artery in the brain) and then death. Arteries are blood vessels that carry blood away
from the heart.
HOW IS AUTONOMIC DYSREFLEXIA TREATED?
The way autonomic dysreflexia is treated is to try to lower the blood pressure by elevating the head and
the upper body at a 45 degree angle (a position between lying on one's back and sitting up straight). The
cause of autonomic dysreflexia then needs to be identified. Most commonly, the cause is an expanded
and irritated bladder. In such a case, the bladder would be drained to relieve the expansion and irritation.
All tight clothing should be removed from the patient because even stimulation of the skin can cause
autonomic dysreflexia. If the symptoms continue to persist, medications to lower blood pressure may be
given. Lowering the blood pressure is so important because high blood pressure can cause an artery (a
blood vessel that carries blood away from the heart) in the brain to burst. The patient needs to be
constantly monitored until the blood pressure, heart rate, and other important bodily functions necessary
to maintain life return to normal.
WHAT ARE OTHER CHARACTERISTICS OF PEOPLE WITH AUTONOMIC DYSREFLEXIA?
Autonomic dysreflexia typically occurs to people with quadriplegia (inability to move and/or feel the arms,
legs, and trunk of the body below the area where a spinal cord injury occurred) and paraplegia (inability to
move and/or feel the legs and lower trunk area). The lower trunk is the area of the stomach and lower
back.
WHY IS IT CALLED AUTONOMIC DYSREFLEXIA?
The word "autonomic," refers to the autonomic nervous system (discussed above). The word "autonomic"
comes from the Greek word, "autos" meaning "self," and the Greek word "nomos," meaning "law." The
word "dysreflexia" comes from the Greek word "dys," which means "bad," and the Latin word, "reflectere,"
meaning "to bend backward," referring to a reflex. So autonomic dysreflexia can roughly be translated to
mean "bad reflexes in the autonomic nervous system."
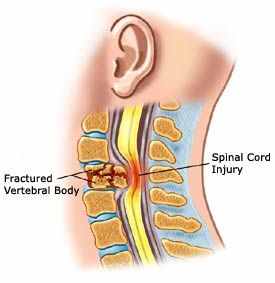
A type of spinal cord injury can
lead to autonomic dysreflexia.














